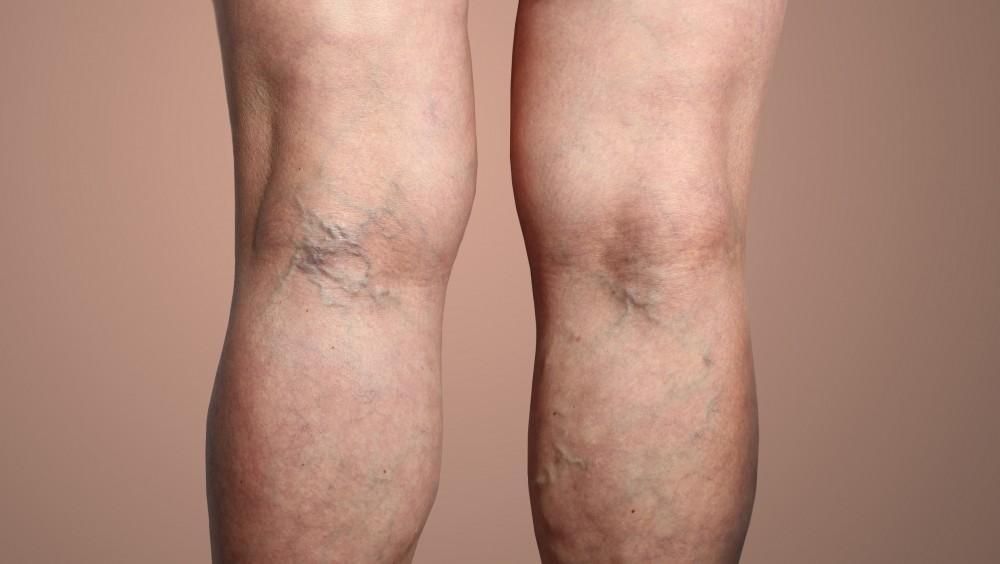
Vein disease may seem cosmetic, yet visible veins often signal impaired blood return and sustained venous pressure. Common signs include heaviness, ankle swelling, night cramps, itching, and skin discoloration near the lower leg. Board certification matters because it reflects formal specialty training, examination, and ongoing professional review. That preparation supports accurate diagnosis, safer procedure planning, and treatment choices that address the actual source of symptoms.
Better First Assessment
A careful first visit often prevents wasted time and incomplete care. Varicose veins affect nearly one in four adults, while chronic venous disease affects a smaller but still meaningful share of the population. Early symptoms can look minor, even when valve failure is already present. Patients may choose El Paso Vein Doc East Side for board-certified treatment when detailed ultrasound mapping, symptom review, and physician oversight are needed before any procedure is selected.
Accurate Source Detection
Surface veins are not always the primary problem. In many cases, reflux in a deeper or connecting vessel creates the pressure that enlarges branches under the skin. Duplex ultrasound helps identify backward flow, vein diameter, and valve weakness before treatment begins. That imaging reduces the chance of treating what is visible while the driving source remains active and continues to trigger aching, swelling, or later return.
Lower Procedure Risk
Safety depends on more than the treatment itself. Patient selection, sterile technique, anesthesia use, and real-time imaging all shape the result. Board-certified physicians are trained to screen for a history of clotting, medication interactions, skin fragility, and bleeding concerns before intervention. Careful planning lowers avoidable complications and supports smoother recovery after ablation, sclerotherapy, or other vein procedures performed in an outpatient setting.
Treatment That Fits Disease Stage
Venous disease does not follow one pattern. Some patients report heaviness after standing, while others develop edema, eczema, or skin thickening near the ankle. Board-certified care helps match therapy to disease stage, symptom burden, and ultrasound findings. That fit matters because limited treatment may leave reflux untreated, while excessive intervention can expose a patient to steps that add risk without meaningful clinical benefit.
Stronger Decisions on Surgery
Vein care has changed over time. Many patients now improve with office-based treatment, allowing walking soon after the visit and less interruption to daily activities. Board-certified specialists can weigh surgery against minimally invasive options with stronger clinical judgment. That distinction matters because an overly aggressive approach may increase bruising, pain, or healing delay without improving long-term control of venous hypertension.
Recurrence Often Has a Reason
Recurrence rarely appears without explanation. Persistent reflux, incomplete mapping, missed tributaries, or weak follow-up can all contribute to the return of bulging veins. Board-certified physicians tend to base treatment on anatomy and flow patterns, rather than appearance alone. By closing the vessel that drives pressure first, they reduce the conditions that allow new branches to enlarge and symptoms to reappear.
Follow-Up Protects Results
Results depend as much on what happens after treatment as on what happens during it. Compression instructions, walking guidance, and repeat ultrasound checks help confirm closure and support healthy venous return. Board-certified teams usually follow a structured recovery plan because healing can change over several weeks. Early review also helps catch clot extension, persistent reflux, or skin irritation before a small issue grows into a larger setback.
Better Care for Complex Patients
Many vein patients carry added medical factors. Obesity, diabetes, prior thrombosis, pregnancy history, or limited mobility can alter healing, timing, and the chance of recurrence. Board-certified specialists are trained to account for those variables during evaluation and planning. That broader clinical perspective helps protect patients whose symptoms reflect more than surface appearance and whose circulation requires closer medical judgment.
Credentials Support Accountability
Board certification does not promise perfect outcomes, yet it adds a meaningful layer of accountability. Physicians must complete approved training, pass specialty examinations, and maintain standards over time. Those requirements offer patients a clearer signal than promotional language alone. In vein care, where symptoms may progress gradually, credible credentials help families distinguish medical oversight from options that lack the same level of scrutiny.
Local Access Matters
Convenient access can influence outcomes more than many patients expect. When evaluation and follow-up are easier to schedule, leg pain, swelling, or skin changes are less likely to be ignored for months. The East Side clinic offers extended weekday hours, Saturday availability, and a record of more than 10,000 treatments. Earlier assessment often leads to simpler planning and fewer complications related to delayed care.
Conclusion
Board-certified vein treatment lowers risk because diagnosis, procedure planning, and follow-up are grounded in specialty training and objective imaging. That same approach also reduces recurrence by identifying the vessel responsible for abnormal pressure before surface veins are treated. For patients with persistent symptoms or visible leg changes, credentials are more than a title. They are a practical safeguard for comfort, recovery, and longer-lasting control.